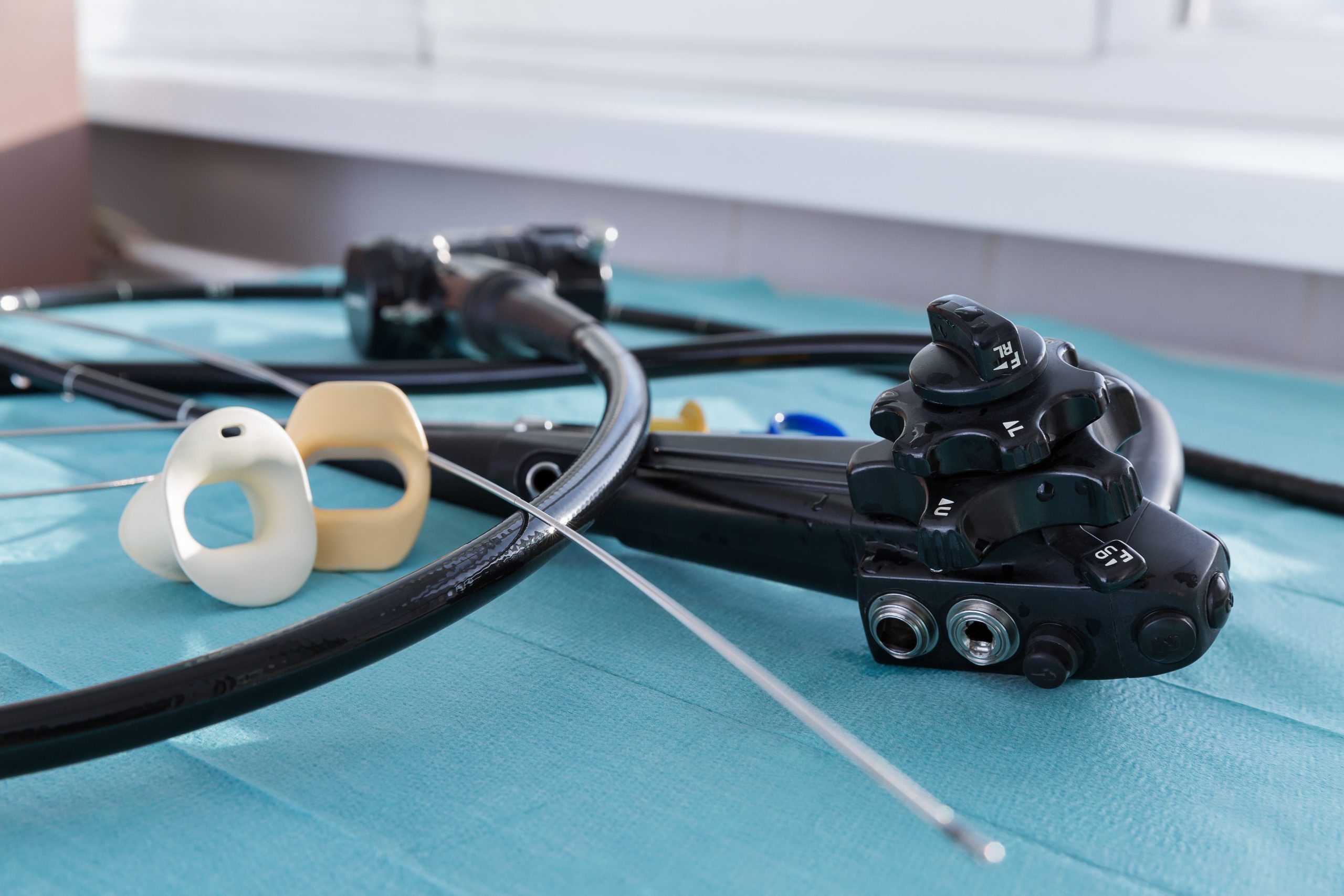
Sterilization vs. High-Level Disinfection
To begin a discussion about the benefits of sterilizing flexible endoscopes versus high level disinfection (HLD), it is first important to understand the key differences between the two. Most importantly, HLD does not fully eliminate all microbes present on the device being disinfected. Specifically, HLD leaves behind a small number of bacterial spores.[1] In contrast, sterilization processes leave no viable microorganisms behind, including spores.
Challenges
One of the key challenges to sterilizing endoscopes is the complexity of the devices. They are highly specialized, made of unique materials, and vary greatly in length. The smallest common flexible endoscope, the rhinolaryngoscope, only has a working length of 300mm long. A colonoscopy, on the other hand, used to visualize and inspect the colon, has a working length of 1680mm, or 1.68m, which is 5.6x longer than the rhinolaryngoscope.[2] The nature of flexible endoscopes creates a series of challenges to sterilization:
- The materials used to manufacture flexible endoscopes are not compatible with steam sterilization
- The complexity of the devices can lead to retention of bio-burden
- The length of the scope or number of working channels can prevent effective low-temperature sterilization
- Sterilization via ethylene oxide requires long exposure and aeration times, is hazardous to personnel and patients, and can interfere with the availability of scopes for scheduled and add-on cases[3]
The above points lend flexible endoscopes, particularly endoscopes used to visualize the gastrointestinal tract, to high level disinfection. As previously discussed, HLD kills the majority of microbes but can leave behind spores.
In the USA, this is acceptable because GI endoscopes are a class 2 medical device. This means they can be processed with HLD since they never contact sterile areas of the body. While this is acceptable, it is not optimal. If leftover spores are introduced into pre-existing wounds or injuries in the GI tract, this can cause infection. Previously, it was thought that GI endoscope infections occurred at a rate of around 1 in 1,000,000. However, a study done by Johns Hopkins found that the rate is actually closer to 1.6 in 1,000.[4] From that data, it is clear that finding a suitable method of sterilization that would eliminate all viable microbes, even in class 2 devices, would benefit both the patient and the facility.
Sterilization
Endoscopes that normally have contact with sterile areas of the body are class 3 devices, and as such must be sterilized before use on patients. Flexible endoscopes used for the GI tract and the airway are class 2 devices, as these parts of the body are not normally sterile, and, as previously discussed, sterilizing class 2 devices would optimize patient safety during procedures that utilize these scopes.
When talking about sterilization of flexible scopes in general, the common method of sterilizing smaller flexible scopes is vaporized hydrogen peroxide (VHP). However, there are specific parameters and criteria that must be met for a flexible scope to be reprocessed via VHP. For example, the Steris VPRO Max can sterilize flexible endoscopes with a single lumen with a diameter > 1mm, but a length < 1050mm, or a scope with two lumens where one lumen has a diameter > to 1mm and a length of < 990mm, and the other lumen has a diameter > 1mm and a length of < 850mm.[5]
This precludes sterilization of the longer GI scopes; as an example, the Olympus HQ-190F colonoscope has a working length of 1680mm. To effectively sterilize these scopes, we are left with ethylene oxide. However, a new technology is emerging that promises to mitigate the issue of length: hydrogen peroxide plus ozone. In this type of sterilizer, VHP is introduced into the chamber and devices are exposed as expected with a traditional VHP sterilizer. However, a second exposure phase that introduces gaseous ozone into the chamber increases the lethality of the process by an additional 1.8 log, and this additional lethality can sterilize devices such as colonoscopes.6 Thus, using ozone in addition to VHP allows a hospital to effectively sterilize class 2 flexible endoscopes, removing all viable microbial life, which in turn renders the scope far safer to use on a patient than if it had been reprocessed with HLD, whether or not that scope comes into contact with sterile tissue. Of course with any sterilization method, the flexible scope should be clean, leak-tested, and completely dry before reprocessing.
We have seen the challenges facing effective flexible scope sterilization. Particularly for the larger gastrointestinal endoscopes, the complexity of the devices makes sterilization difficult, but not impossible. As technology continues to advance, it can only benefit both facilities and patients if we apply the same routine sterilization procedures to all flexible endoscopes, regardless of FDA device classification, just as is done with standard surgical instrumentation.
[1] See The Joint Commission’s HLD BoosterPak at https://www.jointcommission.org/assets/1/6/TJC_HLD_BoosterPak.pdf
[2] Working lengths pulled from Olympus America flexible endoscope specifications, current as of April 21, 2019
[3] See parameters for 100% ETO sterilization for the Olympus TJF-Q180V duodenoscope at https://medical.olympusamerica.com/sites/default/files/pdf/TJF-Q180V_ReprocessingManual.pdf
[4] See the relevant study at https://www.hopkinsmedicine.org/news/newsroom/news-releases/infection-rates-after-colonoscopy-endoscopy-at-us-specialty-centers-are-far-higher-than-previously-thought
[5] Sylvie Dufresne, PhD, and Thomas Richards, PhD, “The First Dual-Sterilant Low-Temperature Sterilization System”, Canadian Journal of Infection Control 31, no. 3 (Fall 2016): 173